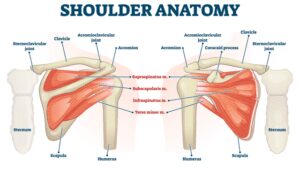
Osteoarthritis is a degenerative disease that affects all joints of the body, especially weight-bearing joints like the knees and hips. The knee is the most commonly affected load-bearing joint where the medial or lateral meniscus (articular cartilage providing shock absorption for the joints) wears down and causes bone-on-bone contact that produces pain.
There is no single factor that has been identified that predisposes an individual to osteoarthritis. Although aging is indeed strongly associated with it, it must be emphasized that aging itself does not cause osteoarthritis, nor should osteoarthritis be considered a “normal” aging process. However, several factors related to aging may contribute to the development.
Osteoarthritis risk factors to consider
1. Age. Strongest risk factor. It can start as a young adult, but the risk increases with age.
2. Gender. Male are more commonly impacted before the age of 45 and females after 45 years old. Hand osteoarthritis is more common in females in particular.
3. Joint Alignment. Abnormal alignment or faulty movement patterns predispose joints to develop osteoarthritis. Repetitive joint injuries, physical labor from work or sports, trauma to any joint, ligament or cartilage tears, and repetitive motion can increase the risk of developing osteoarthritis.
4. Obesity. Also considered as one of the strongest risk factors which cause joint overload.
5. Genetics. Family history of osteoarthritis. Also inherited connective tissue disorders that predispose people to looser ligaments and thus hypermobile joints which can lead to more wear and tear of the cartilage between joints and more rapid development of osteoarthritis.
Signs and Symptoms of Osteoarthritis:
1. Deep, Aching poorly localized pain. This occurs in the affected joint and is relieved by rest.
2. Stiffness. Usually occurs in the morning and after 15 minutes of inactivity/static postures especially sitting. The stiffness in the morning usually improves in about an hour with movement.
3. Joint Pain. Due to the absence of protective cushioning of the joint. May be experienced with changes in the weather especially cold.
4. Crepitus. Due to loss of cartilage and joint surface irregularities, during the early stages of OA, there is fine crepitus which becomes coarse and more pronounced during the last stage of OA.
5. Limited Joint Motion
6. Flares. Acute pain immediately precipitated by trauma or synovitis (inflammation of the membrane surrounding the joint).
7. Effusion. Swelling around the joint affected.
Deformities caused by Osteoarthritis
Hand
- Heberden’s Node – bony swelling on the joints of the fingers closest to the nails and lateral deviations of the fingers.
- Bouchard’s Node – occurs at the joints in the middle of each finger
- Enlargement and radial subluxation of the thumb joint connecting thumb to wrist carpal bones and producing a squared appearance of the hand.
Knee
- Chondromalacia Patella – softening, fissuring and fibrillation of the cartilage where the kneecap angles in the direction depending on the weak side.
- Genu Varum or Bow-Legged – commonly found in osteoarthritis especially of the lateral compartment of the knee.
- Genu Valgus or Knock-kneed – also commonly found in osteoarthritis especially of the medial compartment of the knee.
Hip
- The typical deformity is having a fixed flexion, adduction and external rotation producing apparent shortening of the involved limb so that the person walks with a pronounced pelvic tilt,
lumbar scoliosis, and a flexed contralateral knee. - Other abnormalities are hip dysplasia, slipped capital femoral epiphysis.
Foot
- Bunion – bony swelling of the big toe metatarsophalangeal joint with lateral deviation of the great toe (hallux valgus). It can also be found on the fifth toe.
- Hammer Toe – toes are in flexed posture at the IP (interphalangeal) joints which suggest evidence of spasms and contractures of both flexor and extensor musculature.
The prognosis has little possibility of complete restoration of function. If treatment is started early and is continued faithfully, the pain may be relieved or reduced significantly. The mobility of the hip usually becomes quite restricted, but stiffness is tolerable as long as the pain and deformity are controlled. When a flexion and adduction deformity develops, the disability becomes severe because of postural (apparent) shortening of the leg.
Some treatments or medications are given by doctors. Salicylate not only relieves moderate pain but may also inhibit cartilage deterioration and even exert beneficial effects on the regeneration of the cartilage. Acetaminophen can be used for mild cases. NSAID’s and Opioid Analgesics are used for moderate to severe osteoarthritis. Corticosteroids may also produce temporary pain relief, but should not be repeated too frequently (not more than 3x/year) at a given joint because it has a long-term harmful effect on the articular cartilage.
Physical Therapy as Treatment for Osteoarthritis
Physical therapy management of osteoarthritis include range of motion exercises, gentle mobilization and myofascial release techniques, strengthening exercises to protect and balance the muscular dynamics surrounding osteoarthritic joints, assistive device gait training especially following a joint replacement, joint protection and energy conservation techniques, deep heating modalities for the pain, provision of a home exercise program, and patient/family education.